
Vitiligo Treatment Pathways
Vitiligo treatment options vary depending on factors such as age, type of vitiligo, disease activity, and access to specialist care. This page explains the main treatment options for vitiligo and how they are typically accessed, including NHS and specialist pathways.
For a general overview of vitiligo treatments and supportive care, see our Vitiligo Treatment overview.
Making Treatment Decisions
Available treatments focus on slowing its progress, concealing the white patches or trying to bring about repigmentation, which is unlikely to be complete or permanent. Vitiligo may even get better by itself in up to 50% of affected individuals. This uncertainty about what may happen with vitiligo leaves you with a range of choices about what to do. This is a very personal decision, informed by a number of different issues, such as:
- What you feel about your vitiligo.
- How it is affecting your life.
- What your skin colour means to you.
- How your community responds to your vitiligo, and what would be their reaction to a total change in skin colour?
- Medical risks and side-effects of treatments.
- Availability of non-medical solutions which could help you manage more easily
It can take up to three months before treatments start to work and some people find this waiting for repigmentation very distressing. Treatment may not be the right option for you, or it might be something you pursue alongside camouflage products and counselling or psychological support.

The Different Vitiligo Treatment Pathways
There are many different treatment options for vitiligo, and the best treatment will ultimately depend on your age, what type of vitiligo you’re dealing with, and how fast it’s progressing. We recommend discussing treatment options with your healthcare provider to know which one is best for you.
The following sections outline the main categories of vitiligo treatment options, with links to more detailed guidance for each:
These vitiligo treatment options are accessed through different NHS and specialist pathways. Accessing these treatments can be difficult to navigate. The illustration below shows the diagnosis and treatment journey, and how each treatment may be accessed.
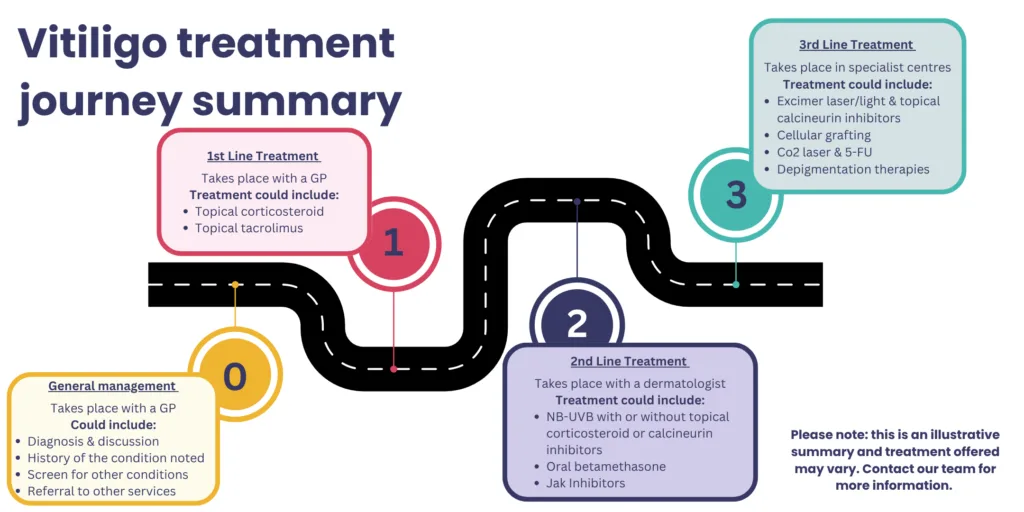
Vitiligo treatment is often approached in stages, sometimes described as first‑, second‑ and third‑line treatments.
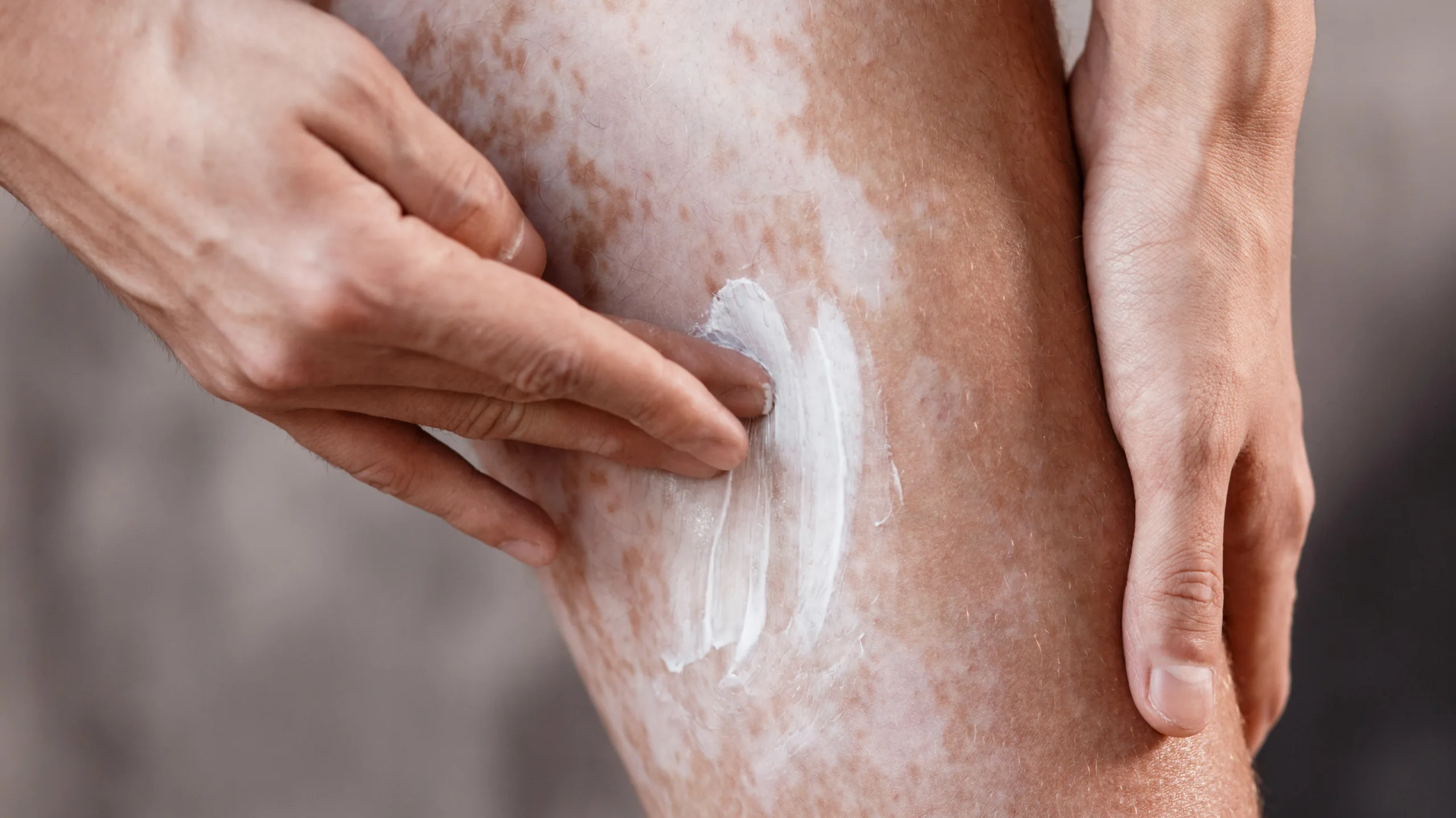
First‑line treatments are usually initiated in primary care and may include topical creams such as corticosteroids or tacrolimus, alongside advice on skin care and sun protection.
Second‑line treatments may require referral to dermatology services and can include options such as light‑based therapies or newer specialist treatments, depending on eligibility and availability.
Third‑line treatments, including surgical procedures or highly specialised therapies, are considered only in selected cases and are typically managed in specialist centres.

How effective are vitiligo treatments?
The effects of treatment vary between individuals. Some people experience significant repigmentation, while others see limited or no response. Treatments may not work on all areas of the body, and repigmentation can relapse over time. Research suggests that treatment response depends less on age than on factors such as:
- where vitiligo appears on the body
- how early treatment begins
- how extensive the affected areas are
Treating vitiligo on the face tends to be more effective than on other body areas. Children often respond better than adults. Small areas are generally easier to treat than larger ones. Bleaching and surgical treatments are used very occasionally and only in specific circumstances.
Should I get a second opinion on my vitiligo treatment?
It is very important that you have confidence in your doctor. If you are concerned that you have not been given sound advice, or you feel that your doctor has not listened to your concerns, you should get a second opinion. Your options are:
- 1. Go back to your doctor to discuss your concerns further: You should do this if you feel that your doctor did not have all the information about your condition. Perhaps you discussed more than one medical problem with them and not enough time was given to the particular problem that bothered you. Possibly you forgot to tell the doctor something important – easy to do if you are anxious! It may be helpful to write a note of everything you want to say next time, or take someone with you to remind you (and give support). This makes it easier for the doctor to give you an opinion based on all the facts available.
- 2. Ask for a second opinion from a doctor in the same GP practice: If your doctor has been given all the information about your condition and you are not satisfied about the response, asking for a second opinion is the best option. A good doctor is not afraid of a second opinion, which might confirm the first diagnosis, or pick up on something that has been missed. Doctors are human – they have to know about a very wide range of illnesses and any individual GP will have more knowledge and skills in some areas of medicine than others.
Remember that you are registered with a Practice and not an individual doctor. The doctors in a Practice share responsibility for their patients and will want to do the best for them, so it is reasonable to ask another doctor there for a second opinion. You may want to ask to speak to the Senior Partner or the Practice Manager for this opinion.
A second opinion may confirm that your GP is absolutely right and your concern is unfounded, but it is also possible that another doctor will have a different opinion. In this case, you will have to decide whether this second opinion is more acceptable to you (a second opinion is not necessarily going to be better than the first).
Can I seek advice from outside my GP practice?
If you feel that you cannot seek a second opinion from another doctor in the Practice, or you have done this and are still concerned, you can get help from your local NHS Patient Advice and Liaison Service (PALS).
Information about this service should be available on all NHS premises. You can also find the contact details and a number to ring for your local PALS on the website www.pals.nhs.uk, or from the ‘Health Services Near You’ directory page on the NHS Choices website. Ask to speak to the PALS Officer, who will be able to help you.
This should be a last resort, if you really feel you have lost confidence in your doctor and cannot consult anyone else in the practice. There is no guarantee another doctor would do anything different or better, so you need to make sure that you want to take this step!
You may find additional evidence‑based information about vitiligo treatment options from the following organisations: NHS guidance on vitiligo & British Association of Dermatologists information on vitiligo treatments.
