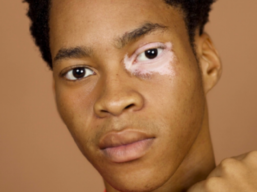
Diagnosis & Assessment
How vitiligo is diagnosed usually involves a clinical assessment by a GP or dermatologist, based on medical history, examination of the skin and the impact of the condition. This page will talk you through the process in detail so you know what to expect, and what support you are entitled to.
How Vitiligo Is Diagnosed
The best way to confirm a diagnosis of vitiligo is to see your doctor. You can even prepare for your visit by doing the following:
- Reviewing your family medical history.
- Making notes concerning any stressful events that have occurred in your life.
- Making a list of chemicals you may have come into contact with.
- Considering taking a friend or family member with you for support.
- Preparing a list of questions to ask your doctor.
During your visit, your doctor will ask several questions concerning various areas of your life including family history and whether you have had any injuries. If available, your patches will be examined using a ‘Woods Lamp’ (ultraviolet lamp) which will assist in narrowing down and eliminating the possibility of it being another skin condition. There are a number of characteristics that healthcare professionals may look out for when diagnosing vitiligo:
- Depigmentation of areas of skin (or hair)
- Characteristic of depigmentation areas including: colour, margins, extent and distributions, location, exhibition of the Koebner Phenomenon and progression.
Your GP may ask you a number of questions such as:
- The number of patches you have and how the patches have progressed
- The impact on your quality of life
- If you are aware of any triggers that may have caused the onset or be making your vitiligo worse
- If you have any family history of vitiligo
They may also carry out an examination taking into account:
- The distribution of your patches
- Presence of the Keobner Phenomenon
- The % of body surface affected
- They may test for associated conditions or your vitamin D level
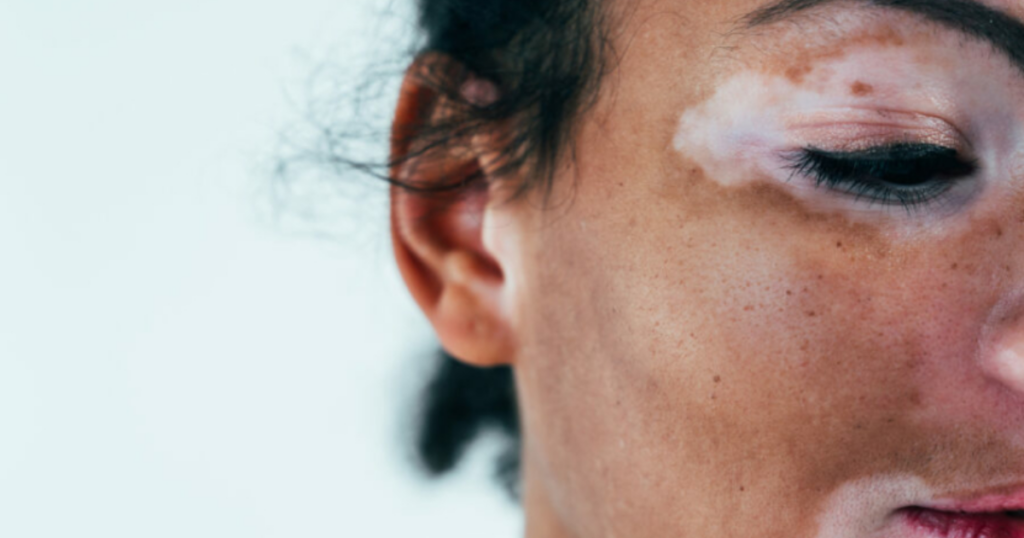
How your GP can help
Understanding how vitiligo is diagnosed can help you prepare for appointments and know what questions to ask. GPs have access to a wide range of resources to help you manage your vitiligo – but with most appointments only lasting about 10 minutes, it’s really important that you are aware of the ways in which your doctor can help. During your appointment you can request different kinds of support from your GP, and we hope this will give you an insight into what you can ask for, and help you prioritise your time during your appointment. Here are the 7 ways in which your GP can help you, at any stage in your vitiligo journey:
- Providing information about vitiligo: GPs can provide you with lots of useful information including what treatments and support services are available in your area.
- The importance of sun protection and vitamin D: Some NHS Trusts may still provide sunscreen on prescription. Your GP can advise on this and also provide advice on sun protection and why it is important for vitiligo. In addition you may consider asking your GP about your vitamin D requirement. The body creates vitamin D from direct sunlight on the skin when outdoors, so when people living with vitiligo avoid the sun or use High SPSF sun protection, this can lead to a deficiency.
- Offer a referral to a skin camouflage service: Skin Camouflage can be a powerful tool in helping you live happily with your vitiligo. A local skin camouflage service may be available through your local dermatology service, your GP can advise on this and make this referral for you.
- Offer psychological support: Your GP has the ability to refer you for emotional and psychological support – don’t be afraid to push to get access to this help at any point in your vitiligo journey.
- Offer treatment options: Your GP can offer you treatment and talk you through your options and what to expect.
- Arrange referral to a dermatologist: If you do not meet the above criteria or you do and have not had success with the prescribed treatment then your GP can arrange a referral to a dermatologist where other treatment options may be discussed.
- Consider any coexisting autoimmune conditions: Certain immune cells and processes that trigger inflammation in vitiligo also play a role in some other conditions, and your GP can check for these conditions and arrange a further investigation if they suspect you may have one.

Receiving your diagnosis: What now?
Being diagnosed with vitiligo can be highly emotional and stressful. No doubt you’ll have a million and one questions rushing through your head. The first thing to remember is that you are by no means alone and there are many groups and information sources out there (and on The Vitiligo Society website here) to help you.
Regarding vitiligo treatments, there are a variety of methods that may help restore pigmentation, although the outcome may not be permanent or even stop the spread of patches.
You may decide that you don’t want or need to try treatment methods. You can discuss the best options with your doctor or dermatologist. An alternative method to concealing white patches on your skin is to use camouflage. Skin camouflages are longer-lasting waterproof creams, designed to blend your vitiligo patches to your natural skin tone. Applications to the face can last 12-18 hours and 2-3 days if applied to the body. This may help if the white spots are causing you to feel self-conscious.
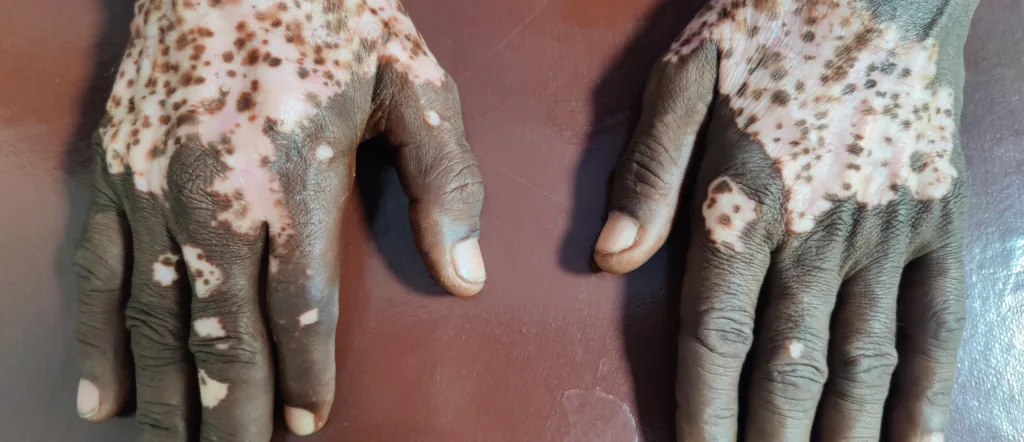
Vitiligo Activity & Stability
Vitiligo does not behave in the same way for everyone. For some people, the condition changes slowly over time, while for others it may remain stable for long periods.
Vitiligo activity refers to whether vitiligo is currently changing. Signs of active vitiligo may include:
- the appearance of new white patches
- existing patches increasing in size
- changes occurring over weeks or months rather than years
Vtiligo stability describes a period during which vitiligo does not appear to be spreading or changing. Many clinicians consider vitiligo to be stable when no new patches have appeared and existing patches have not changed for a sustained period, often six to twelve months or longer.
In rare cases, people may experience spontaneous repigmentation, where colour returns to some areas of skin without treatment. This is unpredictable and not fully understood, and it does not happen for most people with vitiligo. Spontaneous repigmentation may be partial, temporary, or limited to certain areas of the body, and it does not necessarily mean the condition will remain stable long‑term.
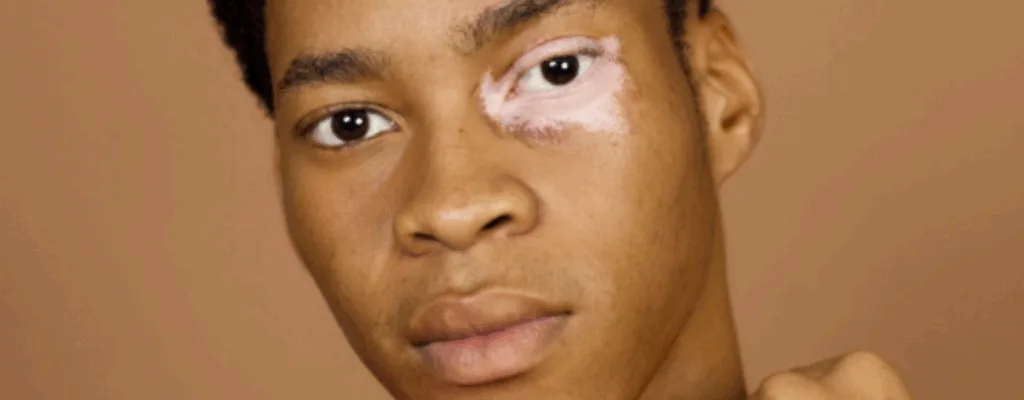
Assessing disease activity and stability can help dermatologists:
- understand how the condition is behaving over time
- discuss appropriate monitoring or treatment options
- set realistic expectations about change
Vitiligo can move between periods of activity and stability, and stability does not guarantee that the condition will not change again in the future. It is also possible for different areas of the skin to behave differently at the same time.
Vitiligo Severity & Impact
The severity of vitiligo is not determined only by how much skin is affected. Small areas of vitiligo can have a significant impact for some people, while more extensive vitiligo may have less impact for others.
Clinicians may consider several factors when assessing severity, including:
- the extent and distribution of depigmented skin
- whether visible areas such as the face or hands are affected
- the rate at which vitiligo is changing
Impact refers to how vitiligo affects a person’s life. Vitiligo can influence:
- confidence and self‑esteem
- emotional wellbeing
- social interactions and relationships
- daily activities or work
Research shows that vitiligo can have a meaningful psychological and social impact, even though it is not physically harmful or contagious. For this reason, understanding impact is just as important as assessing physical changes to the skin.
Assessing severity and impact together helps ensure that care and support are guided by the individual’s experience, not solely by the visible extent of the condition.

When to See a Dermatologist
Many people with vitiligo are first assessed by their GP, who can provide initial guidance and reassurance. In some situations, a referral to a dermatologist may be helpful. Referral may be part of how vitiligo is diagnosed when symptoms are unclear or changing.
You may be referred to, or wish to discuss referral to, a dermatologist if:
- the diagnosis of vitiligo is uncertain
- vitiligo is spreading quickly or changing significantly
- highly visible areas such as the face or hands are affected
- vitiligo is having a noticeable impact on emotional wellbeing, confidence or quality of life
- treatment options need to be reviewed or discussed
- vitiligo is affecting a child or young person

Dermatologists specialise in skin conditions and can help:
- confirm the diagnosis, sometimes using tools such as a Wood’s lamp
- assess disease activity and stability
- discuss treatment options and expected outcomes
- support decision‑making based on individual circumstances
Not everyone with vitiligo needs specialist care, and some people choose not to pursue treatment. However, seeing a dermatologist can provide reassurance, particularly if there are concerns about progression, impact or management options.
If you are unsure whether a referral would be helpful, your GP can discuss this with you and take your preferences into account.
Can I self diagnose vitiligo?
We would always suggest seeking a formal diagnosis of vitiligo from a trained healthcare professional. However, there are some signs and symptoms that you can look out for if considering if you might have vitiligo.
Vitiligo manifests in loss of pigmentation in the skin and/or hair. The patches of depigmentation are usually asymptomatic, but many people report that their patches can be itchy.
The patches may at first appear hypopigmented (low in pigment) and pale before eventually turning white in colour. sometimes the patches may be white in the middle surrounded by a pale area of skin. Patches are usually clear in shape, and their boarders may be smooth or irregular.
Patches can appear anywhere but are more common around the eyes, nostrils, belly button, an genital areas. Sometimes vitiligo can be symmetrical and other times not. Sometimes vitiligo can appear as a result of damage to the skin, known as the Koebner Phenomenon. Hair roots can also be affected, resulting in white eyelashes, brows and hair.
If left untreated patches will usually enlarge and spread over time, although it’s rare that they will cover almost all your skin. It is possible for vitiligo can stabilize over time, without treatment.
Vitiligo and Pregnancy FAQs
Can vitiligo transfer from mother to baby?
There is just one report that we are aware of which describes this happening. It is unclear from that report whether the antimelanocyte antibodies crossed the placenta or whether it was a genetic predisposition that was in play. The answer is that it is possible but probably uncommon, though if the vitiligo is active in the mother, then that might make it more likely to occur.
Can pregnancy cause vitiligo or make it worse?
Pregnancy is likely to be a potential factor in the precipitation of the onset of vitiligo because of the disruption of the immune system that occurs with pregnancy. Additionally, it could be anticipated that pre-existing vitiligo might get worse with pregnancy in some women. According to research conducted in 2021, 17% of participants found that pregnancy caused their vitiligo patches to grow in size or number, where as 12% found reported an improvement to their vitiligo. 71% reported that pregnancy had no affect on their vitiligo.
You can read more about vitiligo, pregnancy and family planning by visiting our blog, The VitLife. If you have a question about vitiligo and pregnancy then please email our team: hello@vitiligosociety.org.uk

Learn More About Vitiligo
Vitiligo Treatments: Treatment options and management
Understanding Vitiligo: Causes, myths and who vitiligo affects Trusted clinical information
You may also find the following NHS‑endorsed sources helpful when learning how vitiligo is diagnosed: NHS overview of vitiligo & British Association of Dermatologists guidance on vitiligo.