New & Approved Treatments
New vitiligo treatments are changing how vitiligo is managed, with recent approvals expanding options for people who have not responded to first‑line care. In recent years, advances in research have led to new therapies that target the immune pathways involved in pigment loss. Some of these treatments have now reached regulatory approval, while others remain under investigation.
This page explains the new and recently approved treatments for vitiligo, how they fit within NHS care pathways, and what this means in practice for people living with the condition.
What is ruxolitinib (Opzelura)
Ruxolitinib represents one of the first new vitiligo treatments to receive NHS approval. Ruxolitinib is a topical medicine that belongs to a group of treatments known as Janus kinase (JAK) inhibitors. JAK inhibitors work by interfering with immune signalling pathways that contribute to inflammation.
In vitiligo, the immune system mistakenly targets melanocytes — the cells responsible for producing skin pigment. By reducing this immune response, ruxolitinib can allow remaining melanocytes to recover and begin producing pigment again.
Ruxolitinib is applied directly to affected areas of skin as a cream, rather than taken orally. This distinguishes it from systemic (whole‑body) JAK inhibitors.
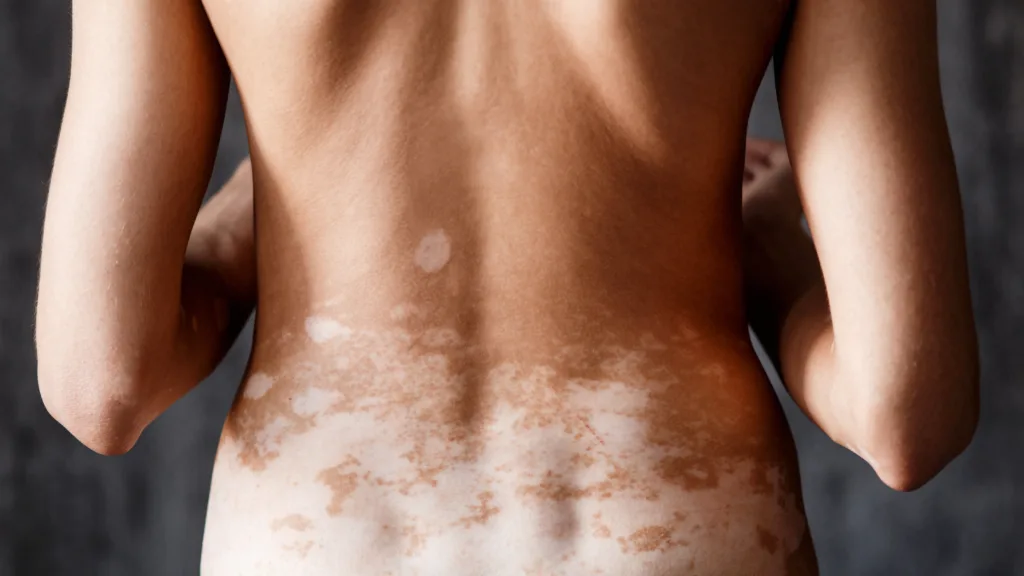
Who is ruxolitinib approved for in the UK?
In the UK, ruxolitinib cream has been approved for NHS use in people who meet specific clinical criteria. It is recommended for:
- People aged 12 years and over
- Non‑segmental vitiligo
- Facial involvement
- Use as a second‑line treatment, when first‑line topical treatments (such as topical corticosteroids or calcineurin inhibitors) have not worked or are not suitable
These criteria reflect the evidence reviewed during regulatory assessment and help ensure the treatment is prescribed safely and appropriately.
How is ruxolitinib accessed on the NHS?
Ruxolitinib is prescribed and monitored within secondary care, meaning it is initiated by a hospital‑based dermatology service rather than by a GP.
Access depends on:
- Referral to a dermatology service
- Assessment against eligibility criteria
- Local NHS implementation pathways
Even after national approval, availability can vary between services as local prescribing arrangements are established. Your dermatologist can advise on whether ruxolitinib is suitable for you and how it is accessed in your area.
What can people expect from treatment?
Ruxolitinib is not a cure for vitiligo. Response varies between individuals.
Clinical studies show that:
- Repigmentation tends to occur gradually over several months
- Facial vitiligo responds more consistently than other body areas
- Continued treatment is often needed to maintain pigment
- Some people will see limited or no response
As with all vitiligo treatments, ongoing review helps guide whether treatment should continue.

Safety and monitoring
Ruxolitinib cream was generally well tolerated in clinical studies. The most commonly reported side effects were:
- Local skin reactions, such as acne or mild irritation
- Itching at the application site
Because the medicine is applied topically, absorption into the bloodstream is low compared with oral JAK inhibitors. However, long‑term safety data is still developing, and treatment should always be supervised by a dermatologist.
Systemic JAK inhibitors: what’s on the horizon
Other new vitiligo treatments are still undergoing regulatory review and are not yet approved for routine use. In addition to topical ruxolitinib, systemic JAK inhibitors — medicines taken orally that work throughout the body — are being studied for vitiligo.
Several systemic JAK inhibitors have shown encouraging results in advanced clinical trials, particularly for non‑segmental vitiligo. These treatments aim to address disease activity more broadly rather than treating individual patches.
At present:
- Systemic JAK inhibitors are not approved in the UK for vitiligo
- Some have been submitted for review by regulatory authorities outside the UK
- Any future NHS use would require separate assessment of safety, effectiveness and cost‑effectiveness
While these developments are promising, systemic treatments carry different risks and monitoring requirements compared with topical therapies. Decisions about their use will depend on robust evidence and regulatory approval.
Where this fits in the treatment pathway
Vitiligo treatment pathways are personalised and depend on factors such as disease activity, extent, location of patches, previous treatment response and individual preference.
For most people, management begins with first‑line topical treatments, such as topical corticosteroids or calcineurin inhibitors. If these treatments are not effective, not suitable, or not tolerated, second‑line options may be considered.
Second‑line treatments can include:
- Light‑based therapies, such as narrowband UVB phototherapy
- Newer approved treatments, such as ruxolitinib (Opzelura), for people who meet specific eligibility criteria
These options are considered alternatives or complements to one another, rather than steps that must occur in a fixed order. The choice between phototherapy, newer topical treatments, or a combination approach is guided by clinical assessment and shared decision‑making between the patient and their dermatologist.
Newly approved treatments expand the options available for people whose vitiligo has not responded to first‑line care, but they do not replace established therapies. Individual suitability, access, and expected benefit all play a role in determining the most appropriate approach.

Looking ahead: The future of vitiligo treatment
The approval of ruxolitinib marks an important step forward for vitiligo treatment. It also signals a shift in how vitiligo is recognised and addressed within healthcare systems.
Research continues into:
- Optimising long‑term outcomes
- Combination approaches
- Identifying which treatments work best for different patterns of vitiligo
As evidence evolves, so too will treatment options. The Vitiligo Society will continue to share clear, evidence‑based updates as further developments emerge.
Learn more about vitiligo treatment
You may also find these pages helpful:
Vitiligo Treatment Options: Overview of available treatments
Topical Vitiligo Treatments: Steroid creams and tacrolimus
Phototherapy for Vitiligo: UVB and PUVA treatment
How Vitiligo Is Diagnosed: Assessment and referral pathways
You may also find the following NHS‑endorsed sources helpful when learning how vitiligo is diagnosed: NHS overview of vitiligo & British Association of Dermatologists guidance on vitiligo.